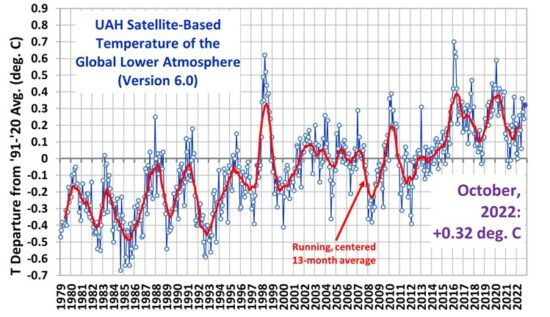
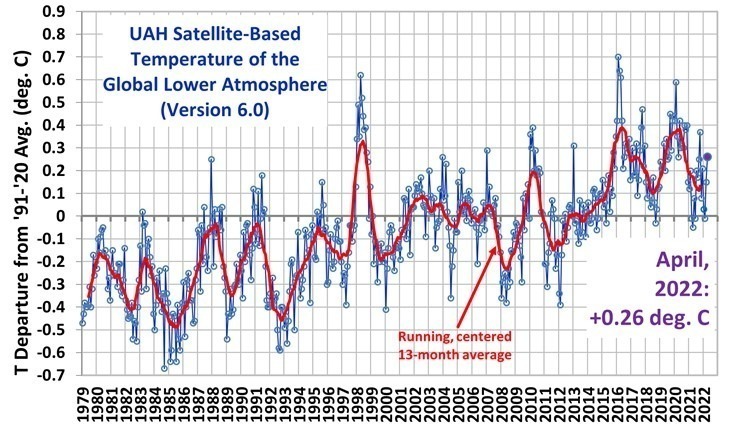
This article from ‘Forbes‘, suggests that an open mind is needed when learning about medical industry practices, research, guidelines, recommendations and trials.
What if doctors kept prescribing drugs based on large clinical trials that had been discredited? That is exactly what is happening in Europe, as guidelines for physicians have remained unchanged even as the studies they are based on were caught up in a two-year-old scandal. Some researchers say thousands of patients may have died as a result in the United Kingdom alone.
Current European Society of Cardiology guidelines recommend that beta-blockers be given to many patients having surgery for noncardiac reasons to protect the heart during surgery. (US guidelines are somewhat less aggressive in their endorsement of perioperative beta-blockade.) The guidelines, which were published in 2009, were based on analyses of the available trials. The strongest evidence came from the DECREASE family of trials, which appeared to strongly support perioperative beta-blockade, and one other large trial, POISE, which raised concerns that beta-blockers might lead to an increase in deaths. When the ESC committee combined all the data they found a neutral effect on mortality but a strong benefit due to significant reductions in non-fatal MI and stroke with beta blocker use. This was the basis for the strong recommendation in the ESC guidelines.
In 2011, however, faith in the reliability of the DECREASE trials was shattered as a result of a scientific misconduct scandal centering on the principal investigator of the studies, the now disgraced Dutch researcher Don Poldermans. The issue was further complicated because, in addition to his key role in the trials, Poldermans was the chairman of the committee that drafted the guidelines.
Now, a group of UK researchers, led by Darrel Francis, have published in the journal Heart the results of a meta-analysis of the remaining non-DECREASE trials that tested perioperative beta-blockade. With the removal of the DECREASE trials the findings were strikingly different from the earlier analyses. In a combined population of 10,529 patients taken from 9 trials there was a statistically significant increase in the risk of death in the group of patients randomized to beta-blockers:
- 162 deaths in 5264 patients randomized to beta-blockeres versus 129 deaths in 5265 patients randomized to placebo, for a 27% increase in the risk of death (RR 1.27, CI 1.01- 1.60, p=0.04).
In sharp contrast, the two randomized placebo-controlled DECREASE studies resulted in a 58% reduction in mortality associated with beta-blockers (although this was not statistically significant).
The analysis did find some benefits associated with beta-blockade, including a statistically significant reduction in non-fatal MI. However, it also found a significant increase in hypotension and stroke. In the new meta-analysis any beneficial effects are clearly overshadowed by the most important finding of an increased risk in death.
Read the complete article, by Larry Husten, Forbes Contributor (I’m a medical journalist covering cardiology news) here.